Prurigo nodularis is a particularly severe skin condition that’s estimated to impact 72 in 100,000 people in the US, although with many cases not being diagnosed or reported, this number could be higher.
This skin disorder can have a huge impact on an individual’s physical and emotional health. However, there’s still a lot we don’t understand about how it’s caused, and therefore, how we should treat it.

We’ve examined the symptoms, causes, management, and prevention strategies associated with this unpleasant disorder. Plus we’ve looked at the importance of clinical research into the condition, and how it will allow us to develop new medical interventions.
Interested in joining a clinical trial for Prurigo Nodularis?
Find and match with clinical trials that suit your needs and eligibility through our platform. Take the first step towards accessing innovative treatments today!
What is prurigo nodularis?
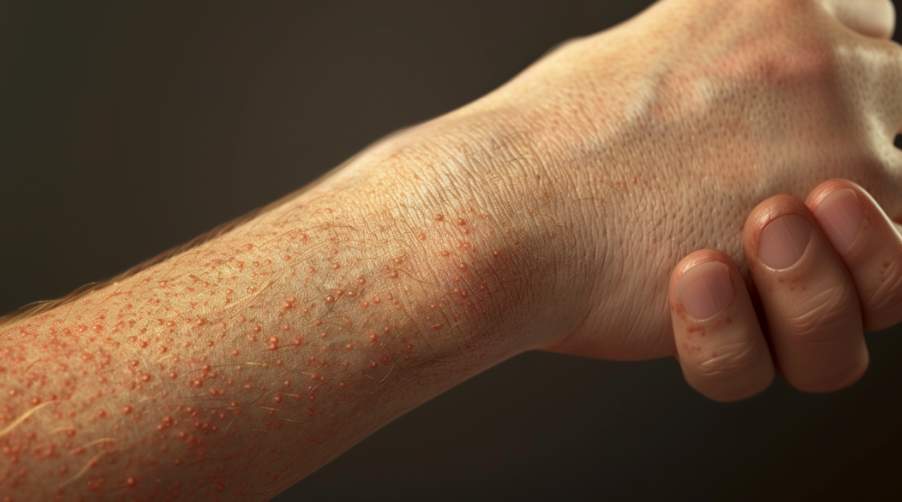
Prurigo nodularis (sometimes known as nodular prurigo or picker’s nodule) is an extremely irritating skin condition that manifests itself as hard, itchy bumps, typically on the arms, legs, abdomen, or back.
Because it can cause such severe and persistent discomfort, it often has an impact on a sufferer’s emotional wellbeing and quality of life, so finding an effective treatment is crucial. Managing the condition and recognising it early can also help avoid further complications.
Who is more likely to get prurigo nodularis?
Although anyone can suffer, population research about prurigo nodularis suggests it is more common among adults aged 40–69, people of African American descent, and slightly more prolific in women, with 54.2% suffering compared with 45.5% of men. Women also tend to experience more severe symptoms.
Your chances of getting it might also increase if you have a skin condition such as eczema, psoriasis, or xerosis cutis. It can also be caused by underlying conditions including HIV, liver disease, thyroid disease, hepatitis C, diabetes, gout, cancer, and certain bacterial, viral, and parasitic infections. Mental health disorders can even be a triggering factor, especially if they lead to compulsive scratching.
Symptoms of prurigo nodularis
Prurigo nodularis appears as hard, raised bumps with a thick crust which are either the same tone as your skin, or can be various shades of red, brown, pink, or black. The condition varies in severity from person to person, with some people having a few nodules, and others suffering from several hundred.
The bumps can be categorized as:
- nodules – more than one cm wide and can appear above, below, or level with the skin surface
- papules – less than one cm wide and only on the skin surface
- plaques – shallow, scaly lesions more than one cm wide but only on the skin surface
The unpleasant physical symptoms include intense itchiness, and occasional burning or stinging. This very often causes people to scratch and pick – which only makes the problem worse. Secondary physical symptoms include scaly lesions, thickened, darkly pigmented areas, and scarring caused by scratching.
Prurigo nodularis can also lead to mental health problems, with one study by the Journal of Investigative Dermatology finding increased risks of self-harm, attention deficit hyperactivity disorder, eating disorders, and schizophrenia.
Causes of prurigo nodularis
The exact cause isn’t known, but prurigo nodularis is thought to stem from a dysregulation of nerve or immune cells in the skin.
Studies of prurigo nodularis, for example, have shown a decrease in nerve fibers in the outer skin layer, but an increase in the deeper layer. However, prurigo nodularis causes can also be associated with a number of other underlying conditions.
Skin conditions
Scratching damaged skin might cause prurigo nodularis, making people with itchy skin conditions particularly prone to it. As such, if you suffer from eczema, dermatitis, cutaneous, T-cell lymphoma, lichen planus, xerosis cutis, keratoacanthomas, or bullous pemphigoid, you may be at a higher risk.
Immune response
The body’s immune response is believed to play a significant role in prurigo nodularis. If it reacts too strongly, it can cause chronic inflammation and immune dysregulation, which might contribute to the formation of nodules and persistent itching.
Nerve changes
Nerve dysfunction may contribute to the formation and persistence of prurigo nodularis. If nerves in the skin are hypersensitive or malfunction, this could lead to intense itching and scratching, which might cause nodules to appear.
Similarly, other nerve-related conditions, such as neuropathic itch or neurogenic inflammation, might also be a causing factor as they contribute to chronic itching and skin changes.
Infections
Viral, bacterial, or fungal infections that make the skin itch could potentially trigger infections. The resulting scratching and rubbing might not only cause prurigo nodularis – it can make existing cases prone to further infections, which can worsen symptoms and delay the healing process.
Kidney disease
People with kidney disease may be more likely to suffer with prurigo nodularis as a result of waste products building up in the blood, mineral imbalances, or chronic inflammation. These individuals are advised to work with their healthcare providers to manage both conditions.
Stress
Stress can significantly impact the immune system and worsen inflammation, which might lead to prurigo nodularis symptoms. It can also encourage behaviors such as persistent picking and scratching, which can cause new nodules to appear. In turn, prurigo nodularis can cause increased stress, which creates a vicious cycle.
Genetics
Several studies link genetic factors with prurigo nodularis, so if family members have it, you may be more likely to get it. The genes involved and the mechanisms influencing the condition are still being investigated. However, it's likely that multiple genetic factors interact with environmental triggers to increase the risk.
How is prurigo nodularis diagnosed
It can be relatively easy to confuse prurigo nodularis with other skin disorders which look similar.
Visiting a dermatologist is usually the first step for a correct diagnosis. Typically this will involve conducting a clinical and microscopic examination of your skin.
This often includes a dermoscopy, which looks at your skin under a powerful microscope. It can also include a biopsy, which involves removing a small sample of skin to examine in a lab. A decrease of nerve fibers in the outer layer and an increase in the dermis are typical findings.
They might also take blood and urine samples to test for underlying diseases that could be the root cause.
What treatments are there for prurigo nodularis?
Prurigo nodularis treatment and management techniques vary depending on the severity of the condition and any underlying conditions. Always seek advice from a healthcare professional before you start a course of treatment.
Injections
Corticosteroid and botulinum toxin injections can reduce itching and inflammation, offering relief and reducing the size of the nodules. Other medicinal injections, such as immunosuppressants or biologics, can target underlying causes such as immune system overactivity, or specific inflammatory pathways.
Topical drugs
Several creams can provide relief from itching and reduce inflammation to help get the condition under control. They include corticosteroid cream, capsaicin cream, calcineurin inhibitors, coal tar, menthol, pramoxine, and emollient-rich moisturizers.
Other therapies
Cryotherapy is often used in combination with corticosteroid injections, and works by freezing off large or especially itchy skin lesions with liquid nitrogen.
Alternatively, phototherapy uses ultraviolet light to calm the immune cells that release histamines, which reduces itchiness and helps lesions heal – although several treatments are usually needed.
Newer treatments
Modern treatments for prurigo nodularis include:
- immunosuppressants, which are especially useful in cases caused by autoimmune conditions such as psoriasis and lupus
- naloxone and naltrexone, which can help manage itching by blocking certain receptors involved in itch signals
- medications such as gabapentin and pregabalin, which can reduce neuropathic itching and discomfort
- thalidomide (a last-resort option due to the risks of significant side effects) which can modulate the immune response and reduce inflammation
Home remedies
If you want to complement the treatments suggested by your healthcare professional, you could try an ice pack or cold compress to temporarily reduce the irritation. Having a lukewarm bath infused with colloidal oatmeal, which has natural anti-inflammatory properties can also help to soothe your skin and combat itching.
Regularly applying petroleum jelly or a hypoallergenic cream will keep skin hydrated, repair it, and can reduce itching and irritation. You should also use fragrance-free soaps and skincare products which are specifically designed for sensitive skin.
Possible complications of prurigo nodularis
If prurigo nodularis isn’t managed effectively, it can lead to further difficulties which can cause even more stress and discomfort, so it’s important to have a treatment plan in place.
These complications include scarring, skin discoloration, scratch marks, and thickened skin due to persistent scratching. Local infections can also occur where the skin has become damaged and broken.
Sleep disturbance can also result from the chronic itching the condition causes. Plus there are psychological implications, including anxiety, depression, and a reduced quality of life.
Some long-term treatments, such as steroids, can also have their own side-effects, such as skin thinning or stretch marks.
How to prevent prurigo nodularis
Preventing prurigo nodularis can be difficult as it likely arises from a combination of factors, and the causes aren’t fully understood. However, there are a few steps you can take to minimize the risks of getting it or making it worse.
Protection in the sun and the heat
Excessive exposure to the sun can cause skin irritation and flare-ups, so always wear a broad-spectrum sunscreen with at least SPF 30, and try to avoid direct sunlight when it’s at its strongest.
It’s also wise to avoid becoming overheated and sweating as this can also be a contributing factor, so wear breathable fabrics in the heat and try to avoid activities that cause too much perspiration.
Personal hygiene
Keep your fingernails short and filed smooth to prevent accidental damage to the skin caused by scratching, and to avoid carrying unwanted bacteria that can cause a secondary infection.
It’s also important to cleanse regularly, but avoid any skincare products and soaps that contain harsh chemicals, fragrances or alcohol, and stick with products designed specifically for sensitive skin.
Stress management
If stress is contributing to your prurigo nodularis, take the time to incorporate relaxation techniques such as meditation, yoga, and mindfulness into your daily routine.
We also recommend speaking to a healthcare professional for advice about how to reduce stress, anxiety, or depression that is either caused by your prurigo nodularis, contributing to it, or both.
Physical barriers
If you already suffer from an irritating skin condition, wearing long sleeves and gloves can stop you from scratching, which might then prevent prurigo nodularis from occurring. You can also try using oils and ceramides as a barrier, but speak to your dermatologist or a doctor first.
Clinical research and findings for prurigo nodularis
There has been an increase in research into the pathophysiology, treatment, and epidemiology of prurigo nodularis in recent years. This aims to improve the management and diagnosis of the condition, and enhance the quality of life for patients.
This will be welcome news to anyone suffering from this debilitating condition, and some clinical trials for prurigo nodularis are actively seeking new participants.
Types of research
Different types of research are undertaken to make different discoveries about prurigo nodularis, all with the aim of advancing medical interventions and improving patient lives.
For example, epidemiological studies about prurigo nodularis examine the number of cases and where they occur within various populations and geographic regions. This helps establish risk factors and population-specific characteristics.
Clinical trials about prurigo nodularis assess the effectiveness and safety of new treatments and interventions, which might include biologics, immunosuppressants, topical agents, and systemic therapies. Find out more about participating in clinical trials to discover whether this is something you might want to consider.
Observational studies about prurigo nodularis meanwhile, look at the condition’s history alongside patient experiences – including quality of life, long-term outcomes, and treatment satisfaction.
Advances in understanding prurigo nodularis
Importantly, these studies help shed new light into prurigo nodularis so scientists can gain a better understanding about its causes, effects, and treatments. For example:
- studies suggest there’s a genetic predisposition to prurigo nodularis, although more research is needed to determine the specific genes and mechanisms
- research has highlighted the role of immune system dysregulation in prurigo nodularis, including the involvement of cytokines, T cells, and other immune responses
- examinations into the neurological aspects of prurigo nodularis – such as the role of nerve growth factors and neurogenic inflammation – have enables scientists to focus on treatments that target nerve-related pathways
- studies on skin barrier function and prurigo nodularis suggest that disruptions to the skin’s surface can make the condition worse
Implications for treatment and management
The findings from clinical research into prurigo nodularis will help the medical and scientific community advance their understanding of its underlying mechanisms so they can provide the best possible interventions.
This might include developing new pharmacological agents, biologic therapies, or medical devices that target both the causes and symptoms, and devizing personalized approaches that are tailored to unique patient needs.
Ultimately, this research could save an enormous amount of suffering, and improve the quality of life for thousands of people across the world.
Conclusion
Prurigo nodularis is a deeply unpleasant condition that causes an immense amount of discomfort, and can lead to mental health problems for sufferers due to the persistent itching, scarring, and chronic nature.
The exact causes are not fully understood, which is why clinical research into its epidemiology is crucial so we can understand how to treat, diagnose and manage it better, and stop it from recurring.
If you think you’re suffering from prurigo nodularis, it’s vital that you seek help from a medical professional who can take the appropriate tests, diagnose it properly, and put a personalized treatment plan in place. They will also be able to help you treat any underlying health conditions that might be a causing factor.
FAQs
Is prurigo nodularis an autoimmune disease?
Prurigo nodularis isn’t classed as an autoimmune disease, but inflammation does play a role, and immune-modulating therapies are sometimes used to treat it. It’s more accurately described as a complex dermatologic disorder.
Can prurigo nodularis kill you?
As a condition in itself, prurigo nodularis isn’t life-threatening. However, the impact it can have on a persons’ quality of life should not be underestimated, and it can lead to significant psychological distress. Severe cases and complications may also require more serious medical interventions.